Helicobacter pylori in Alaska Natives
(Redirected from Dyspepsia – H. Pylori)
Helicobacter pylori is present in the stomach of the majority of adult Alaska Natives, with a similar prevalence in other circumpolar indigenous peoples (such as in Canada, Greenland, Russia, etc). The high prevalance, high drug resistance rate, and high reinfection rate present unique challenges for management of Alaska Natives with dyspepsia symptoms.
Background
Research
A substantial amount of research has been published regarding this topic. As of October 2017, PubMed search for (alaska[Title] OR polar[Title] OR arctic[Title]) AND helicobacter[Title] returned 29 articles. In June of 2016 researchers from the CDC presented Grand Rounds at YKHC and gave this excellent talk which summarized current knowledge.
International Multi-Disciplinary Working Group
In 2016 an international, multi-disciplinary working group, including representatives from the CDC Arctic Research Center and Alaska Native Tribal Health Consortium, published an Expert Commentary[1] which thoroughly reviews the epidemiology, associated clinical syndromes, diagnosis, and treatment of H. pylori in high prevalence populations. Some of the key findings/recommendations were:
- The test-and-treat strategy (using serology, urea breath test, stool antigen test, other techniques) should not be used in high prevalence populations (such as in Alaska Natives).
- "When treatment is employed, treatment should consist of regimens that have evidence of high efficacy after taking into consideration the antimicrobial resistance patterns in the region."
- Evidence supports treatment of H. pylori only in these situations:
- Duodenal ulcer
- Gastric ulcer
- MALT lymphoma
- "When the goal is treatment of dyspepsia in patients from populations where H. pylori is highly prevalent, there is moderate evidence that H. pylori therapy should be undertaken only when there is endoscopic or histopathological confirmation of a condition associated with improvement following elimination of H. pylori, such as peptic ulcer disease."
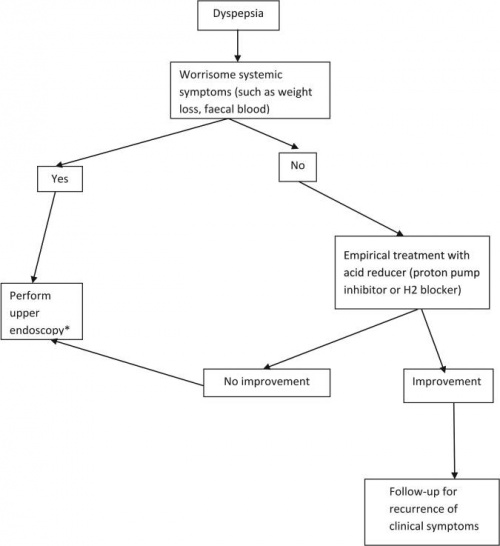
Based upon these conclusions, the Working Group proposed the following algorithm for management of dyspepsia in high prevalence (>60%) populations (this includes Alaska Natives):
Controversies
Evidence is equivocal regarding treatment of H. pylori in the setting of severe gastritis which is not associated with NSAID or EtOH use.[1] Please note that severe gastritis is an endoscopic diagnosis. Endoscopists may differ in their management of this diagnosis.
H. pylori Culture and Sensitivities
H. pylori culture with sensitivities (from endoscopic biopsy specimens) is unavailable in most health care settings. Fortunately, the CDC provides this service for rural, high prevalence Alaska communities, and YKHC participates in this program. Results take 1 to 2 months, so a particular patient's results have little utility in treating his/her infection. But population results inform the local H. pylori Antibiogram which should be utilized when prescribing H. pylori treatment.
Pediatric Considerations
The management algorithm is the same for adult and pediatric patients. However, local pediatric EGD's are only available for teens who are essentially adult size.
SUMMARY
- Substantial research supports a different diagnostic and treatment algorithm for H. pylori in high prevalence populations.
- When dyspepsia fails to respond to a PPI, patients should be referred for EGD.
Resources
- CDC Slide ShowUpdates on H. Pylori Research in Alaska 2016
- Dyspepsia (H. pylori) YKHC Clinical Guideline
ANMC H. Pylori Treatment Guidelines
- Nov 2016 (Archive)
- Feb 19, 2020 (Archive)
YKHC Clinical Guidelines
Common/Unique Medical Diagnoses
References
- ↑ 1.0 1.1 McMahon BJ, Bruce MG, Koch A, et al. The diagnosis and treatment of Helicobacter pylori infection in Arctic regions with a high prevalence of infection: Expert Commentary. Epidemiology and Infection. 2016;144(2):225-233. doi:10.1017/S0950268815001181. Free PMC Article.