Transcutaneous paCO2 Monitoring: Difference between revisions
From Guide to YKHC Medical Practices
m (AndyS moved page Trancutaneous pCO2 Monitoring to Trancutaneous paCO2 Monitoring) |
|||
| (10 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
Transcutaneous CO<sub>2</sub> (TC-CO<sub>2</sub>) monitors function by measuring the CO<sub>2</sub> which diffuses out the skin. Modern TC-CO<sub>2</sub> monitors are a highly accurate, non-invasive method for estimating paCO<sub>2</sub>.<ref>Nassar BS, Schmidt GA. [https://doi.org/10.1513/AnnalsATS.201701-034FR '''Estimating Arterial Partial Pressure of Carbon Dioxide in Ventilated Patients: How Valid Are Surrogate Measures?'''] Ann Am Thorac Soc. 2017 Jun;14(6):1005-1014. doi: 10.1513/AnnalsATS.201701-034FR. PMID: 28570147.</ref><br> | Transcutaneous CO<sub>2</sub> (TC-CO<sub>2</sub>) monitors function by measuring the CO<sub>2</sub> which diffuses out the skin. Modern TC-CO<sub>2</sub> monitors are a highly accurate, non-invasive method for estimating paCO<sub>2</sub>.<ref name="Nassar2017">Nassar BS, Schmidt GA. [https://doi.org/10.1513/AnnalsATS.201701-034FR '''Estimating Arterial Partial Pressure of Carbon Dioxide in Ventilated Patients: How Valid Are Surrogate Measures?'''] Ann Am Thorac Soc. 2017 Jun;14(6):1005-1014. doi: 10.1513/AnnalsATS.201701-034FR. PMID: 28570147.</ref><br> | ||
<br> | |||
[[File:Sentec.PNG|left]] | |||
<br clear=all> | |||
<br> | <br> | ||
== Primary Purpose == | == Primary Purpose == | ||
YKDRH obtained TC-CO<sub>2</sub> monitors for the purpose of | YKDRH obtained TC-CO<sub>2</sub> monitors for the purpose of monitoring paCO<sub>2</sub> <u>trends</u> in patients receiving high-flow nasal cannula or non-invasive ventilation (i.e. CPAP/BiPAP). This was necessary because end-tidal CO<sub>2</sub> monitoring is not compatible with these interventions. | ||
| Line 9: | Line 12: | ||
# Applicable for all age groups (including extremely premature neonates). | # Applicable for all age groups (including extremely premature neonates). | ||
# Initial reading requires approximately five minutes to establish. | # Initial reading requires approximately five minutes to establish. | ||
# TC-CO<sub>2</sub> | # TC-CO<sub>2</sub> is '''substantially more accurate''' than peripheral venous CO<sub>2</sub> for estimating paCO<sub>2</sub>.<ref name="Nassar2017"/> | ||
# Because CO<sub>2</sub> takes several minutes to diffuse out of the skin, the displayed TC-CO<sub>2</sub> reading at any given time reflects the paCO<sub>2</sub> from 2-4 minutes prior. | |||
# The tracing is a flat line (rather than the waveform created by exhaled air). | |||
# TC-CO<sub>2</sub> is used to follow paCO<sub>2</sub> trends; it DOES NOT measure instantaneous levels. Therefore, TC-CO<sub>2</sub> '''IS NOT''' an acceptable substitute for ET-CO<sub>2</sub> in situations such as: | |||
## Confirmation of ET-tube placement. | ## Confirmation of ET-tube placement. | ||
## CPR (neither for CPR adequacy nor ROSC identification). | |||
## Respiratory monitoring during sedation. | ## Respiratory monitoring during sedation. | ||
## Any situation where apnea is a | ## Any situation where monitoring for apnea or any rapid changes in paCO<sub>2</sub>. | ||
# The accuracy of end-tidal CO<sub>2</sub> as an estimate of paCO<sub>2</sub> is largely dependent upon how closely a patient's lung function matches an ideal lung. For patients who are intubated for non-respiratory issues, their lung function should pretty closely approximate an ideal lung, and thus end-tidal CO<sub>2</sub> should estimate paCO<sub>2</sub> with reasonable accuracy. But for patients with lung processes which create V/Q mismatches, end-tidal CO<sub>2</sub> is not a good estimate of paCO<sub>2</sub>. In such situations, TC-CO<sub>2</sub> provides a MUCH MORE ACCURATE estimate paCO<sub>2</sub>.<ref name="Nassar2017"/> Thus, if paCO<sub>2</sub> requires monitoring in patients with ARDS, bronchiolitis, pneumonia, etc., TC-CO<sub>2</sub> should be considered regardless of the type of respiratory support the patient is receiving (i.e. none, high-flow, or intubated). In such a situation, an intubated patient might be monitored with end-tidal CO<sub>2</sub> to watch for apnea and TC-CO<sub>2</sub> to assess adequacy of ventilation over time. | |||
<br> | |||
== Device == | == Device == | ||
YKDRH has acquired the '''Sentec''' Digital Monitoring System.<br> | YKDRH has acquired the '''Sentec''' Digital Monitoring System.<br> | ||
The Sentec devices provides monitoring of: | The Sentec devices provides monitoring of: | ||
# Instantaneous oximetry | # Instantaneous oximetry (with an adjustable duration trend line) | ||
# Instantaneous heart rate | # Instantaneous heart rate (with an adjustable duration trend line) | ||
# | # Delayed paCO<sub>2</sub> (with an adjustable duration trend line) | ||
== Resources == | == Resources == | ||
: [https://yk-health.org/wiki/File:Transcutaneous_CO2_monitor_SDMS_InstructionManual_EN.pdf Sentec Instruction Manual] | : [https://yk-health.org/wiki/File:Transcutaneous_CO2_monitor_SDMS_InstructionManual_EN.pdf Sentec Instruction Manual] | ||
'''Instructional Videos:''' | '''Instructional Videos:''' | ||
: [https://www.youtube.com/watch?v=7d7XNtQNllA | : [https://www.youtube.com/watch?v=7d7XNtQNllA Sensor Application Neonatal for the Sentec Digital Transcutaneous Monitoring System] | ||
: [https://www.youtube.com/watch?v=7HX7dgqieaM Sensor Application Adult Cheek for the Sentec Digital Transcutaneous Monitoring System] | : [https://www.youtube.com/watch?v=7HX7dgqieaM Sensor Application Adult Cheek for the Sentec Digital Transcutaneous Monitoring System] | ||
: [https://www.youtube.com/watch?v=7PeoOWAtWss Sensor Application Adult Upper Arm for the Sentec Digital Transcutaneous Monitoring System] | |||
: [https://www.youtube.com/watch?v=DLWEH-2VHZc Changing the Sensor Membrane for the Sentec Digital Transcutaneous Monitoring System] | |||
: [https://www.youtube.com/watch?v=zCc4JZsfKZM Sentec Digital Transcutaneous Monitoring System Demonstration] | |||
<br> | <br> | ||
'''PubMed Searches:''' | |||
: [https://pubmed.ncbi.nlm.nih.gov/?term=(%22transcutaneous%20co2%22%5BTitle%5D%20OR%20%22transcutaneous%20carbon%20dioxide%22%5BTitle%5D)%20AND%20(infant%5BTitle%5D%20OR%20neonat*%5BTitle%5D%20OR%20child*%5BTitle%5D) ("transcutaneous co2"[Title<nowiki>]</nowiki> OR "transcutaneous carbon dioxide"[Title<nowiki>]</nowiki>) AND (infant[Title<nowiki>]</nowiki> OR neonat*[Title<nowiki>]</nowiki> OR child*[Title<nowiki>]</nowiki>)] | |||
<br> | <br> | ||
== REFERENCES == | == REFERENCES == | ||
<references /> | <references /> | ||
Latest revision as of 00:14, 31 March 2023
Transcutaneous CO2 (TC-CO2) monitors function by measuring the CO2 which diffuses out the skin. Modern TC-CO2 monitors are a highly accurate, non-invasive method for estimating paCO2.[1]
Primary Purpose
YKDRH obtained TC-CO2 monitors for the purpose of monitoring paCO2 trends in patients receiving high-flow nasal cannula or non-invasive ventilation (i.e. CPAP/BiPAP). This was necessary because end-tidal CO2 monitoring is not compatible with these interventions.
Important Points
- Applicable for all age groups (including extremely premature neonates).
- Initial reading requires approximately five minutes to establish.
- TC-CO2 is substantially more accurate than peripheral venous CO2 for estimating paCO2.[1]
- Because CO2 takes several minutes to diffuse out of the skin, the displayed TC-CO2 reading at any given time reflects the paCO2 from 2-4 minutes prior.
- The tracing is a flat line (rather than the waveform created by exhaled air).
- TC-CO2 is used to follow paCO2 trends; it DOES NOT measure instantaneous levels. Therefore, TC-CO2 IS NOT an acceptable substitute for ET-CO2 in situations such as:
- Confirmation of ET-tube placement.
- CPR (neither for CPR adequacy nor ROSC identification).
- Respiratory monitoring during sedation.
- Any situation where monitoring for apnea or any rapid changes in paCO2.
- The accuracy of end-tidal CO2 as an estimate of paCO2 is largely dependent upon how closely a patient's lung function matches an ideal lung. For patients who are intubated for non-respiratory issues, their lung function should pretty closely approximate an ideal lung, and thus end-tidal CO2 should estimate paCO2 with reasonable accuracy. But for patients with lung processes which create V/Q mismatches, end-tidal CO2 is not a good estimate of paCO2. In such situations, TC-CO2 provides a MUCH MORE ACCURATE estimate paCO2.[1] Thus, if paCO2 requires monitoring in patients with ARDS, bronchiolitis, pneumonia, etc., TC-CO2 should be considered regardless of the type of respiratory support the patient is receiving (i.e. none, high-flow, or intubated). In such a situation, an intubated patient might be monitored with end-tidal CO2 to watch for apnea and TC-CO2 to assess adequacy of ventilation over time.
Device
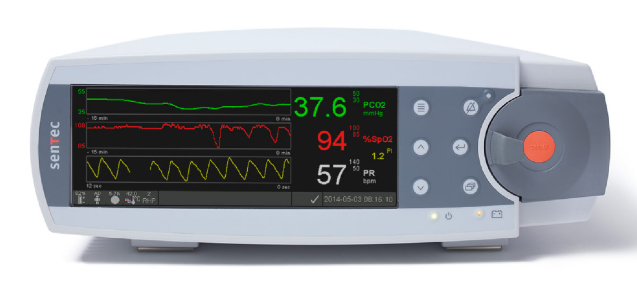
YKDRH has acquired the Sentec Digital Monitoring System.
The Sentec devices provides monitoring of:
- Instantaneous oximetry (with an adjustable duration trend line)
- Instantaneous heart rate (with an adjustable duration trend line)
- Delayed paCO2 (with an adjustable duration trend line)
Resources
Instructional Videos:
- Sensor Application Neonatal for the Sentec Digital Transcutaneous Monitoring System
- Sensor Application Adult Cheek for the Sentec Digital Transcutaneous Monitoring System
- Sensor Application Adult Upper Arm for the Sentec Digital Transcutaneous Monitoring System
- Changing the Sensor Membrane for the Sentec Digital Transcutaneous Monitoring System
- Sentec Digital Transcutaneous Monitoring System Demonstration
PubMed Searches:
REFERENCES
- ↑ 1.0 1.1 1.2 Nassar BS, Schmidt GA. Estimating Arterial Partial Pressure of Carbon Dioxide in Ventilated Patients: How Valid Are Surrogate Measures? Ann Am Thorac Soc. 2017 Jun;14(6):1005-1014. doi: 10.1513/AnnalsATS.201701-034FR. PMID: 28570147.