Sexually Transmitted Infections
We have a lot of STI’s in the Delta region and Alaska typically ranks number one or two in the nation for Chlamydia infections. Due to high levels of STIs, it is recommended that we aggressively screen all females and males over the age of 12.
When someone asks for a STI check, please do urine, self-vaginal or cervical swab, an anal swab, RPR, and HIV tests. Ask if they are interested in Hep B, C and Herpes (HSV1/HSV2) testing as well. When doing the urine STI test, it needs to be done with dirty urine without wiping beforehand. Use the AMB STI PowerPlan which has all testing, treatments, etc.
All positive STI tests will go to the Community Case Manager (CCM) to fill out the required Partner Information forms and follow-up with the patient regarding treatment. The provider should order any required medications and send a message to the CCM.
We use Expedited Partner Therapy for anyone who is positive for GC or CT screening. The EPT kits can be given out at the hospital or the village clinic. Ideally, a Partner Notification Sheet is filled out so public health knows who was treated, but the patient does not need to provide the names of her/his partners. The Community Case Manager is usually able to elicit the partner’s names, even if you are not.
Treatment Recommendations
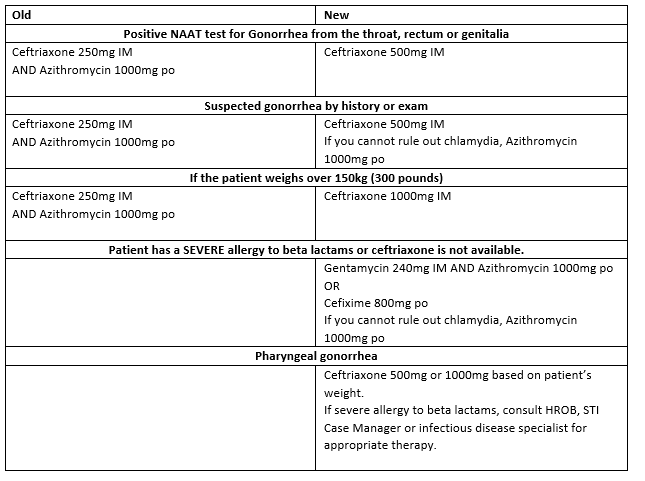
As of July 15, 2021, STI treatment has been modified (see the table below):
Comments:
- While the CDC recommends Doxycycline if chlamydia cannot be ruled out, the STI team believes there is high risk for treatment failure with a 7-day course of medication and that one dose of azithromycin is a better choice.
- There is no effective therapy for pharyngeal gonorrhea beside ceftriaxone, thus we recommend you contact HROB, the STI case manager or an ID specialist. Contacting the experts in Seattle for a recommendation for therapy is highly recommended.
- The recommended medications are on formulary at all of the village clinics and SRCs. They are also in the Pyxis in the ED, Outpatient Clinic, Inpatient and OB.
Please direct any comments or questions to Claire Lewis or David Compton via email or TigerText.
Frequently Asked Questions
- What if the patient is allergic to a recommended antibiotic choice?
- Contact Dr. Compton or an infectious disease specialist at ANMC. Be absolutely sure that the patient is truly allergic. If they are TRULY allergic to all penicillins and cephalosporins, give Azithromycin 2gm orally. It is very important to treat with 2 drugs if possible. If you are not sure, call one of the above for guidance.
- What if the patient is only a contact?
- Get the appropriate testing for STIs. Do a pharyngeal, genital, and anal test as needed. Treat for the appropriate STI as a contact. DO NOT treat their partners.
- Has the patient been previously treated? How can I tell?
- Please check the MAR, medications and notes for evidence of treatment. Make sure that you set the filter on your medications for All Medications All Statuses. Make sure that you set the MAR dates to include the dates in questions.
- When do you recommend an HIV or RPR?
- If the patient has a negative HIV and RPR within the past 6 months they do not need a repeat. We want to strongly encourage those without a recent test to get tested.
- What if the patient answers yes to anal or oral sex? Do I change the treatment?
- If the patient answers yes to having anal or oral sex, perform the appropriate swabs or find a provider to help. They will need to be state lab tests. Treat with the azithromycin and/or Cefixime. Wait for a positive test to treat with different medications.