ANMC ADULT Procalcitonin (PCT) Utilization Guideline/Clinical Pathway
Scope of Guideline
- This guideline is ONLY intended for use in ADULT patients (>18 y/o) and for utilization in the evaluation of procalcitonin levels in patients with the disease states indicated below (i.e. lower respiratory tract infections (LRTI) and sepsis).
- Decisions regarding antimicrobial therapy should NOT be based solely on procalcitonin serum concentrations, but rather should be evaluated in the clinical context of each patient scenario while considering the possible site of infection, likelihood of bacterial infection, severity of illness, and other pertinent clinical data.
Background The Infectious Diseases Society of America (IDSA) estimates that roughly 50% of inpatient antibiotic utilization is inappropriate.1 One clinical scenario included in this estimate is the inappropriate administration of antibiotics to patients without bacterial illness. For instance, approximately 90% of cases of acute bronchitis are caused by viruses; however, roughly two-thirds of all patients presenting with this illness in the United States will receive antibiotics.(2) Given this trend, an increasing national interest has been taken in diagnostic aids which may increase accuracy in the diagnosis of acute bacterial illnesses in order to reduce the unnecessary utilization of antibiotics and, thus, minimized unintended consequences associated with their use (i.e. adverse drug reactions, development of C. difficile infection, development of resistance, etc.). Within this context, procalcitonin has been extensively studied as a biomarker, primarily as an aid in the diagnosis of sepsis and LRTIs. Utilization of the procalcitonin has been associated with a decrease in antimicrobial utilization without a compensatory worsening of clinical outcomes.(3-14)
Procalcitonin (PCT)(15-20)
Amino acid precursor of calcitonin which, under normal circumstances, is produced by thyroid C-cells
- Extra-thyroidal neuroendocrine tissue production increases in response to bacterial infection
- Superior sensitivity when compared to C-reactive protein for the diagnosis of bacterial infection
- Negligible rise of serum levels in response to localized, viral, or intracellular bacterial infections
Kinetics:
- Normal physiologic serum concentrations are <0.1 mcg/L
- Levels rise within 2-4 hours of onset of infection
- Peak levels observed at 8-24 hours / Half-life = 24 hours
Levels are not typically effected by immunosuppression
Cost to patient of a procalcitonin level at ANMC = $116.00
Situations where elevation of PCT may be due to non-bacterial causes (i.e. false positive):
- Massive stress (e.g. severe trauma, surgery (specifically abdominal), cardiogenic shock, burns)
- Treatment with agents which stimulate cytokines (OKT3, anti-lymphocyte globulins, alemtuzumab, IL-2, granulocyte transfusion).
- Conditions that allow “translocation” of intestinal bacteria: (e.g, transiently (24 hrs) after general anesthesia, severe congestive heart failure, profound hypotension regardless of the etiology, end stage liver disease among others).
- Malaria and some fungal infections
- Prolonged, severe cardiogenic shock or organ perfusion abnormalities
- Some form of vasculitis and acute graft vs. host disease
- Paraneoplastic syndromes due to medullary thyroid and small cell lung cancer
Situations where PCT levels may be low when true bacterial infection exists (i.e. false negative):
- Early course of infection
- Localized infection (e.g. pharyngitis, sinusitis, cystitis)
- Subacute infectious endocarditis
- Mycoplasma pneumoniae or Chlamydiophila pneumoniae infection
- Typical PCT levels are slightly higher than those observed during viral illness, but lower than observed during bacterial illness due to other bacterial pathogens.
Procalcitonin Exclusions (5, 7, 17-20)
- Age <18 y/o
- Pregnancy/breastfeeding
- CrCl <30 ml/min or hemodialysis
- Severe immunosuppression (e.g. receipt of immune modulators, neutropenia (ANC <500), transplant patients, or HIV patients with CD4 <200)
- Severe trauma, burn, or major surgery within previous 24 hours (particularly abdominal surgery)
- Chronic infections necessitating antibiotics (e.g. endocarditis, osteomyelitis, tuberculosis)
- Cystic Fibrosis
- Small cell lung cancer or medullary thyroid cancer
- Receipt of OKT-3 and/or anti-thymocyte globulin
- End-stage cancer
Availability, Ordering, and Reporting
Procalcitonin will be available for ordering 24 hours/day and 7 days/week. Test results will typically be available within 2 hours for routine lab orders. The Antimicrobial Stewardship (ASP) pharmacist at ANMC will routinely follow-up on any PCT values resulting during ASP business hours (Monday-Friday 0700-1530).
Note: PCT is a dynamic biomarker and is most useful when trends are analyzed over time in accompaniment with other clinical data. Clinical judgment must be applied to each case and interpretation should always be based on both the tables available in this guideline and clinical context.
Procalcitonin Use in LRTI (3-9, 15-16)
With LRTI being the most common indication for antimicrobial prescription in the northwestern hemisphere and given concern pertaining to overuse of antimicrobials, additional tools are warranted to help clinicians differentiate between bacterial and viral illness. Sufficient data exists indicating that procalcitonin is a useful diagnostic aid in the management of patients with LRTIs including pneumonia, exacerbations of chronic bronchitis, and other assorted lower respiratory tract infections such as acute exacerbations of chronic obstructive pulmonary disease (COPD). A meta-analysis published in 2011 that included 8 studies and 3431 patients found that procalcitonin utilization was associated with a 31% decrease in antibiotic prescriptions and a decrease in antibiotic duration of 1.3 days. Additionally, procalcitonin levels may correlate with the severity of the community-acquired pneumonia (CAP), with patients with procalcitonin levels >10 ng/mL being more likely to have severe disease and/or associated bacteremia.
Based on the above data it is reasonable to consider sending a PCT level on patients with suspected community-acquired, bacterial LRTI (CAP, COPD exacerbation, or bronchitis) who are being considered for initiation of antibiotics. It should be noted that this pathway is intended for use ONLY in community-acquired LRTI. See the below Table 1 for recommended schedule and interpretation of procalcitonin levels for patients with suspected bacterial LRTI.
Table 1: Procalcitonin Utilization in LRTI. INITIAL PROCALCITONIN LEVEL (DRAWN ON ADMISSION)
| PCT Result: | ≤0.1 ng/mL | 0.1 - 0.25 ng/mL | >0.25 – 0.5 ng/mL | >0.5 ng/mL |
|---|---|---|---|---|
| Antimicrobial Recommendation: | Strongly Discouraged | Discouraged | Encouraged | Strongly Encouraged |
| Overruling the Algorithm: | Consider overruling algorithm and initiating antimicrobials if patient is clinically unstable (hemodynamic or | respiratory instability) or at high risk for adverse outcomes (PSI class IV-V, CURB-65 >3, or GOLD III-IV) | N/A | N/A |
| Follow-up/Other Comments: | Reassess patient’s status and repeat | PCT in 6-24 hours if warranted.(*) | Recheck PCT level every 2-3 days to consider early cessation of antibiotics using the above breakpoints or, if initial values >5-10 ng/mL, when a 90% reduction is seen from peak values. | If procalcitonin is rising or unchanged at repeat, consider possibility of treatment failure and workup need for expanded antimicrobial coverage and/or further diagnostic
evaluation. |
PCT = Procalcitonin
(*)Repeat procalcitonin levels should be considered in patients NOT started on antibiotics where no clinical improvement is observed at 6-24 hours and in patients in whom the algorithm is overruled (i.e. initially with low procalcitonin levels who are started on antimicrobials due to clinical instability or risk for adverse outcomes).
Procalcitonin Use in Sepsis (10-16, 21)
Several studies have been performed using procalcitonin to guide antimicrobial therapy in sepsis. These studies have been evaluated in three systematic reviews and meta-analysis. The results show a decrease in antimicrobial exposure of 19-38% without resultant increase in mortality, length of stay, or relapsed/persistent infections. Despite the quantity of primary literature available assessing the use of procalcitonin to guide durations of therapy, there is very little clinical data available to suggest that procalcitonin may serve as a marker to aid with the decision whether or not to start antimicrobials in septic patients. PCT level do appear to correlate with the severity of illness (i.e. sepsis vs. severe sepsis vs. septic shock).
Initial Level (10, 15)
Given the available evidence, it is reasonable to consider obtaining procalcitonin levels at baseline in septic patients in order to help trend levels and evaluate patient improvement or further need for antimicrobials at 48-72 hours of therapy. Delaying antimicrobial therapy in septic patients has a large impact on mortality, and current data showing that PCT levels may be helpful in the decision regarding whether or not to initiate therapy is lacking. Thus, initial PCT levels should NOT be used in this capacity. Clinical judgment and a global patient assessment should be used when making decisions as to whether or not to begin antibiotics in a patient with possible sepsis.
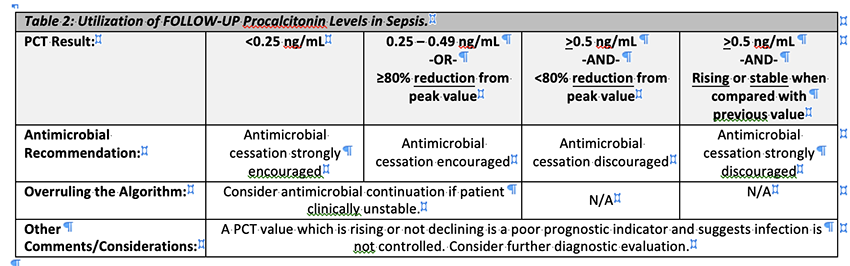
Follow-up Levels (11-16)
Procalcitonin levels should be repeated daily for 3 days, as appropriate, and overall trending of values should be utilized, in combination with culture data and patient specific clinical data, to assess response to therapy and guide antimicrobial duration as per Table 2 below. If an infectious source is identified, the ANMC antimicrobial stewardship program recommends treating with guideline recommended durations of therapy. The below table should be utilized in patients with “sepsis of unknown origin” in which no clear source is identified.
- Dellit TH, Owens RC, McGowan JE Jr, et al. Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America guidelines for developing an institutional program to enhance antimicrobial stewardship. Clin Infect Dis. 2007; 44:159-77
- Albert RH. Diagnosis and management of acute bronchitis. Am Fam Physician. 2010;82(11):1345-1350.
- Christ-Crain M, et al. Procalcitonin guidance of antibiotic therapy in community-acquired pneumonia (ProCAP).
- Am J Respir Crit Care Med. 2006;174:84-93.
- Christ-Crain M, et al. Effect of procalcitonin-guided treatment on antibiotic use and outcome in lower respiratory tract infections: a cluster randomized single blind intervention trial. Lancet. 2004;363:600-7.
- Schuetz P, et al. Effect of procalcitonin-based guidelines vs standard guidelines on antibiotic use in lower respiratory tract infections. JAMA. 2009;302(10):1059-1066.
- Stolz D, Antibiotic treatment of exacerbations of COPD – a randomized, controlled trial comparing procalcitonin- guidance with standard therapy. Chest. 2007;131:9-19.
- Schuetz P, Amin D, Greenwald JL. Role of procalcitonin in managing adult patients with respiratory tract infections. Chest. 2012;141(4):1063-1073.
- Hui L, Luo YF, Blackwell TS, Xie CM. Meta-analysis and systematic review of procalcitonin-guided therapy in respiratory tract infections. Antimicrob Agent Chemother. 2011;55(12):5900-5906.
- Schuetz P, et al. Procalcitonin to initiate or discontinue antibiotics in acute respiratory tract infections. The Cochrane Library. 2012. Issue 9.
- Bouadma L, et al. Use of procalcitonin to reduce patients’ exposure to antibiotics in intensive care units (PRORATA trial): a multicenter randomized controlled trial. Lancet. 2010;375:463-74.
- Nobre V, et al. Use of procalcitonin to shorten antibiotic treatment duration in septic patients. Am J Respir Crit Care Med. 2008;177:498-505.
- Agarwal R, Schwartz DN. Procalcitonin to guide duration of antimicrobial therapy in intensive care units: a systematic review. Clin Infect Dis. 2011;53:379-87.
- Heyland DK, et al. Procalcitonin for reduced antibiotic exposure in the critical care setting: a systematic review and an economic evaluation. Crit Care Med. 2011;39:1792-9.
- Kopterides P, et al. Procalcitonin-guided algorithms of antibiotic therapy in the intensive care unit: a systematic review and meta-analysis of randomized controlled trials. Crit Care Med. 2010;38:2229-41.
- Procalcitonin (PCT) Guidance. (n.d.). Retrieved October 26, 2015, from http://www.nebraskamed.com/careers/education-programs/asp/procalcitonin-pct-guidance
- Schuetz P, Albrich W, Mueller B. Procalcitonin for diagnosis of infection and guide to antibiotic decision: past, present, and future. BMC Medicine. 2011;9:107-15.
- Kibe S, Adams K, Barlow G. Diagnostic and prognostic biomarkers of sepsis in critical care. J Antimicrob Chemother. 2011;66(2):ii33-ii40.
- Simon L, et al. Serum procalcitonin and C-reactive protein levels as markers of bacterial infection: a systematic review and meta-analysis. CID. 2004;39:206-17.
- Grace E, Turner RM. Use of procalcitonin in patients with various degrees of chronic kidney disease including renal replacement therapy. CID. 2014;59(12):1761-7.
- Zazula R, Prucha M, Tyll T, Kieslichova E. Induction of procalcitonin in liver transplant patients treated with anti- thymocyte globulin. Critical Care. 2007;11(6):R131
- Carr JA. Procalcitonin-guided antibiotic therapy for septic patients in the surgical intensive care unit. J Intensive
- Care. 2015;3(1):36.
- Ammar AA, Lam SW, Duggal A, et al. Compliance with procalcitonin algorithm antibiotic recommendations for patients in medical intensive care unit. Pharmacotherapy. 2017;37(2):177-186